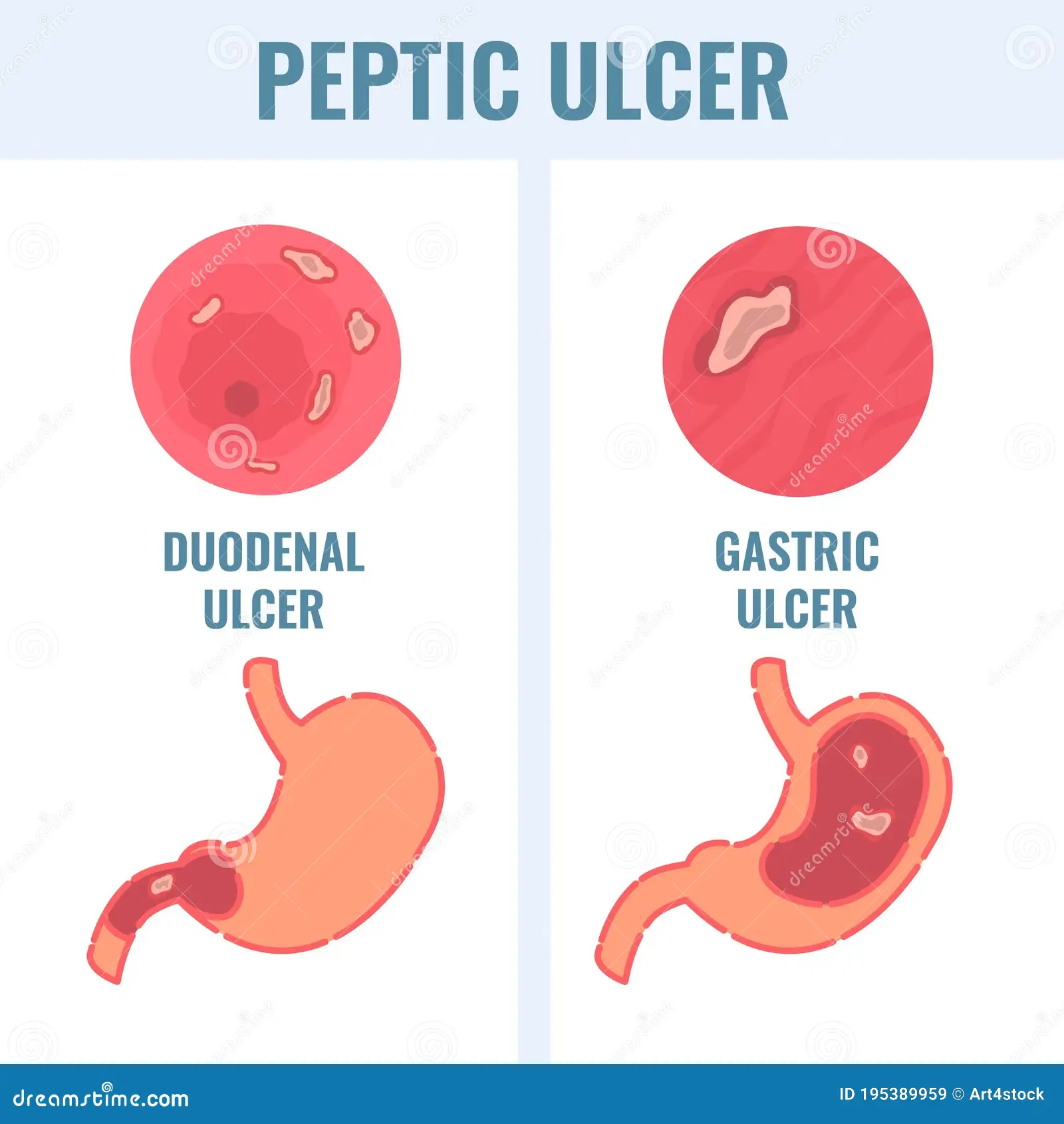
Overview Of Gastric and duodenal ulceration
Gastric and duodenal ulceration refers to the formation of open sores or lesions in the lining of the stomach (gastric ulcer) or the upper part of the small intestine, called the duodenum (duodenal ulcer). These ulcers develop when the protective mucus layer of the stomach or duodenum is compromised, allowing the digestive acids to erode the underlying tissue. Gastric ulcers occur in the stomach, while duodenal ulcers form in the duodenum. These ulcers are often associated with symptoms like stomach pain, bloating, indigestion, and, in some cases, bleeding. The condition can range from mild to severe, with complications such as perforation (a hole in the stomach or intestinal wall), bleeding, or obstruction. While both conditions share similar causes and risk factors, duodenal ulcers tend to cause pain that improves after eating, while gastric ulcers often worsen after meals.
Symptoms of Gastric and duodenal ulceration
- The symptoms of gastric and duodenal ulcers can vary depending on the location and severity of the ulcer, but common symptoms include:
- Abdominal Pain: A burning or gnawing pain in the stomach, usually located in the upper middle or upper left part of the abdomen. The pain may be aggravated by an empty stomach (common in duodenal ulcers) or after eating (common in gastric ulcers).
- Bloating and Fullness: A feeling of bloating, belching, or early satiety (feeling full after eating a small amount of food).
- Indigestion: Persistent indigestion, often described as discomfort or a sense of heaviness in the stomach after eating.
- Nausea or Vomiting: Nausea and vomiting may occur, especially in cases of severe ulceration.
- Heartburn: A sensation of burning in the chest, typically due to acid reflux, may accompany ulcers, particularly gastric ulcers.
- Bleeding: In severe cases, ulcers can bleed, leading to symptoms such as black or tarry stools (melena) or vomiting blood (hematemesis).
- Loss of Appetite: People with ulcers may experience a reduced appetite due to discomfort or pain while eating.
- Unexplained Weight Loss: This can occur in cases of severe or untreated ulcers, especially when associated with bleeding or malnutrition.
Causes of Gastric and duodenal ulceration
- The primary causes of gastric and duodenal ulceration are an imbalance between the protective factors of the stomach lining and the aggressive effects of stomach acids. The main causes include:
- Helicobacter pylori Infection: The bacterium Helicobacter pylori is a significant cause of both gastric and duodenal ulcers. It disrupts the mucus layer that protects the stomach and duodenum from acidic digestive juices, leading to ulceration.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Long-term use of NSAIDs, such as ibuprofen or aspirin, can weaken the protective mucus lining of the stomach and duodenum, increasing the risk of ulcers.
- Excessive Alcohol Consumption: Chronic alcohol use can irritate the stomach lining and increase acid production, leading to ulcer formation.
- Smoking: Smoking contributes to increased acid production and reduces the healing ability of gastric and duodenal ulcers, promoting their development.
- Stress: While stress alone is not a direct cause, it can exacerbate the development of ulcers, especially in individuals who are predisposed to the condition.
- Genetic Factors: A family history of ulcers can increase the risk of developing gastric or duodenal ulceration.
- Other Factors: Conditions like Zollinger-Ellison syndrome, where the body produces excessive stomach acid, can lead to ulcer formation, though this is less common.
Risk Factors of Gastric and duodenal ulceration
- Several factors increase the likelihood of developing gastric or duodenal ulceration, including:
- Helicobacter pylori Infection: A significant risk factor for both types of ulcers. It is estimated that up to 60% of people with peptic ulcers are infected with H. pylori.
- Chronic NSAID Use: Regular use of NSAIDs or corticosteroids significantly increases the risk of ulcer development by weakening the stomach's protective mucus layer.
- Tobacco Smoking: Smoking reduces the stomach's ability to heal ulcers and increases acid production, raising the risk of developing ulcers.
- Excessive Alcohol Consumption: Alcohol irritates the stomach lining and promotes the secretion of stomach acids, contributing to ulcer formation.
- Stress: Although not a direct cause, chronic stress or trauma can exacerbate symptoms and promote the development of ulcers, especially in predisposed individuals.
- Age: Older adults are at a higher risk, particularly those who use NSAIDs regularly or who have an H. pylori infection.
- Family History: A genetic predisposition to gastric and duodenal ulcers increases the risk, as those with a family history of peptic ulcers are more likely to develop them.
- Poor Diet: A diet high in spicy foods, caffeine, or acidic foods may irritate the stomach lining, increasing ulcer risk in susceptible individuals.
Prevention of Gastric and duodenal ulceration
- Preventing gastric and duodenal ulceration involves managing risk factors and adopting healthy lifestyle practices:
- Avoiding NSAIDs: Using pain relievers like acetaminophen instead of NSAIDs can reduce the risk of ulcer formation. If NSAIDs are necessary, they should be used at the lowest effective dose and for the shortest duration possible.
- Eradicating H. pylori: If diagnosed with an H. pylori infection, completing the prescribed antibiotic regimen can help prevent the recurrence of ulcers.
- Limiting Alcohol and Smoking: Reducing or eliminating alcohol consumption and smoking can help protect the stomach lining and reduce acid production.
- Healthy Diet: A diet high in fiber and low in spicy, acidic, or fried foods can protect the stomach and duodenum from irritation.
- Stress Management: Reducing stress through relaxation techniques like yoga, meditation, or exercise can help prevent ulcers from developing or worsening.
- Regular Medical Check-ups: For those at higher risk of ulcers, such as individuals with a family history or those on long-term NSAID therapy, regular check-ups and screenings can help identify issues early before complications arise.
Prognosis of Gastric and duodenal ulceration
- The prognosis for gastric and duodenal ulcers is generally favorable with appropriate treatment. In cases caused by H. pylori infection, successful eradication of the bacteria and acid suppression therapy leads to healing in most patients. Most ulcers can be healed with a combination of medication and lifestyle changes. However, complications such as bleeding, perforation, or gastric outlet obstruction can occur in severe cases, requiring immediate medical intervention. If left untreated, chronic ulcers can lead to scarring and long-term digestive issues. With treatment, recurrence of ulcers can often be prevented, particularly by addressing underlying causes like H. pylori infection or NSAID use. The overall prognosis is highly dependent on the timely initiation of appropriate therapy and avoidance of risk factors.
Complications of Gastric and duodenal ulceration
- Without proper treatment, gastric and duodenal ulcers can lead to several serious complications, including:
- Bleeding: Ulcers that erode blood vessels can cause significant bleeding, which may present as black, tarry stools (melena) or vomiting blood (hematemesis). Severe bleeding may require transfusions or endoscopic interventions.
- Perforation: In severe cases, the ulcer may penetrate through the stomach or duodenal wall, causing a hole (perforation). This can lead to peritonitis (infection of the abdominal cavity), which is a medical emergency.
- Gastric Outlet Obstruction: Ulcers, especially in the duodenum, can cause swelling or scarring that obstructs the passage of food and digestive juices, leading to vomiting, bloating, and weight loss.
- Penetration into Adjacent Organs: In rare cases, ulcers can penetrate into nearby organs like the pancreas or liver, causing further complications.
- Increased Risk of Gastric Cancer: Chronic gastric ulcers, particularly those caused by H. pylori infection, may increase the risk of developing gastric cancer, though this is relatively rare.
Related Diseases of Gastric and duodenal ulceration
- Gastroesophageal Reflux Disease (GERD): A condition where stomach acid frequently flows back into the esophagus, causing heartburn and potential damage to the esophageal lining.
- Irritable Bowel Syndrome (IBS): A functional gastrointestinal disorder that can cause symptoms like bloating, diarrhea, and abdominal pain, often coexisting with gastric or duodenal ulcers.
- Gastric Cancer: Chronic gastric ulcers, especially those caused by H. pylori infection, may increase the risk of developing stomach cancer.
- Peptic Strictures: Chronic ulcers, especially duodenal ulcers, can lead to narrowing of the duodenum, causing digestive issues and obstruction.
- Zollinger-Ellison Syndrome: A rare condition characterized by tumors that cause excessive acid production, leading to multiple ulcers in the stomach and duodenum.
Treatment of Gastric and duodenal ulceration
Treatment for gastric and duodenal ulcers aims to relieve symptoms, heal the ulcer, and prevent complications. Common treatment strategies include: 1. **Antibiotics**: If an H. pylori infection is present, antibiotics are prescribed to eradicate the bacteria and prevent ulcer recurrence. Common antibiotics include clarithromycin, amoxicillin, and metronidazole. 2. **Proton Pump Inhibitors (PPIs)**: Medications such as omeprazole, esomeprazole, or pantoprazole reduce stomach acid production, helping to heal the ulcer and relieve pain. 3. **H2-Receptor Antagonists**: Drugs like ranitidine or famotidine may be used to decrease acid production, although they are less effective than PPIs. 4. **Antacids and Cytoprotective Agents**: Medications like sucralfate protect the ulcerated area by forming a protective barrier over the ulcer, and antacids neutralize stomach acid to relieve pain. 5. **Discontinuing NSAIDs**: If NSAID use is contributing to the ulcer, discontinuation or substitution with alternative pain management strategies may be necessary. 6. **Lifestyle Modifications**: Avoiding alcohol, smoking, and foods that irritate the stomach can promote healing. 7. **Surgical Intervention**: In rare cases, when ulcers cause severe complications such as perforation, bleeding, or obstruction, surgery may be required to remove the ulcer or repair the damaged area.
Generics For Gastric and duodenal ulceration
Our administration and support staff all have exceptional people skills and trained to assist you with all medical enquiries.

Cimetidine
Cimetidine

Ranitidine
Ranitidine

Dexlansoprazole
Dexlansoprazole

Esomeprazole Magnesium Trihydrate BP
Esomeprazole Magnesium Trihydrate BP

Amoxicillin + Clarithromycin + Rabeprazole Sodium kit
Amoxicillin + Clarithromycin + Rabeprazole Sodium kit

Amoxicillin + Clarithromycin + Lansoprazole Kit
Amoxicillin + Clarithromycin + Lansoprazole Kit

Bismuth Subcitrate
Bismuth Subcitrate

Clarithromycin + Metronidazole + Lansoprazol
Clarithromycin + Metronidazole + Lansoprazol

Esomeprazole Sodium Injection
Esomeprazole Sodium Injection

Lansoprazole
Lansoprazole

Nizatidine
Nizatidine

Omeprazole
Omeprazole

Pantoprazole Sodium Sesquihydrate
Pantoprazole Sodium Sesquihydrate

Rabeprazole
Rabeprazole

Cimetidine
Cimetidine

Ranitidine
Ranitidine

Dexlansoprazole
Dexlansoprazole

Esomeprazole Magnesium Trihydrate BP
Esomeprazole Magnesium Trihydrate BP

Amoxicillin + Clarithromycin + Rabeprazole Sodium kit
Amoxicillin + Clarithromycin + Rabeprazole Sodium kit

Amoxicillin + Clarithromycin + Lansoprazole Kit
Amoxicillin + Clarithromycin + Lansoprazole Kit

Bismuth Subcitrate
Bismuth Subcitrate

Clarithromycin + Metronidazole + Lansoprazol
Clarithromycin + Metronidazole + Lansoprazol

Esomeprazole Sodium Injection
Esomeprazole Sodium Injection

Lansoprazole
Lansoprazole

Nizatidine
Nizatidine

Omeprazole
Omeprazole

Pantoprazole Sodium Sesquihydrate
Pantoprazole Sodium Sesquihydrate

Rabeprazole
Rabeprazole